December 2021
Morton’s Neuroma and Location of Pain
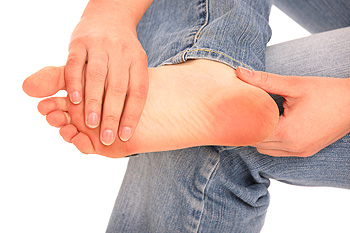 The foot condition that is known as Morton’s neuroma may also be referred to as Morton's syndrome. It is defined as a compressed nerve, and the pain that is felt is generally located between the third and fourth toes. Pain may also consist of a tingling sensation, similar to pins and needles, or numbness on the inside of the two toes. This condition can be caused from wearing shoes that do not fit correctly, or from participating in running and jumping activities. The healing process can bring mild relief, and this includes resting the affected foot as often as possible. It may be beneficial to wear protective pads inside the shoes as they can provide adequate support. If you have developed pain in this area of your foot it is suggested that you schedule an appointment with a podiatrist who can properly diagnose and treat Morton’s neuroma.
The foot condition that is known as Morton’s neuroma may also be referred to as Morton's syndrome. It is defined as a compressed nerve, and the pain that is felt is generally located between the third and fourth toes. Pain may also consist of a tingling sensation, similar to pins and needles, or numbness on the inside of the two toes. This condition can be caused from wearing shoes that do not fit correctly, or from participating in running and jumping activities. The healing process can bring mild relief, and this includes resting the affected foot as often as possible. It may be beneficial to wear protective pads inside the shoes as they can provide adequate support. If you have developed pain in this area of your foot it is suggested that you schedule an appointment with a podiatrist who can properly diagnose and treat Morton’s neuroma.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Thomas Madden of Advanced Foot Care Center. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Killeen, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
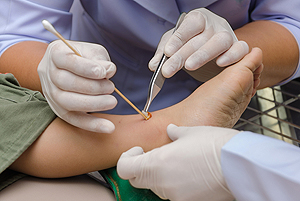
Wounds That Don't Heal Need to Be Checked
What Are Hammertoes?
Hammertoes are painful deformities that frequently form on the second, third, or fourth toe. The condition is often caused by an issue in foot mechanics. This can be caused by the person’s specific gait or the manner in which they walk, or by shoes that do not comfortably fit the deformity. Hammertoes can be formed after wearing shoes that are too narrow or short for the foot or have excessively high heels. Shoes that are not properly sized will force the toes into a bent position for long periods of time. This can cause the muscles to shorten and toes to bend into the deformity of a hammertoe.
Hammertoe can also be caused by complications from rheumatoid arthritis, osteoarthritis, trauma to the foot, heredity, or a cerebral vascular accident. Pain and difficult mobility of the toes, deformities, calluses, and corns are all symptoms of a hammertoe.
Someone who suspects they have the symptoms of a hammertoe should consult with a physician—particularly a podiatrist. Podiatrists diagnose and treat complications of the foot and ankle. If the podiatrist discovers that the affected toes are still flexible, treatment for the hammertoe may simply involve exercise, physical therapy, and better-fitting shoes. Treatment for hammertoes typically involves controlling foot mechanics, such as walking, through the use of customized orthotics.
For more serious cases in which the toes have become inflexible and rigid, surgery may be suggested. During the operation, the toe would receive an incision to relieve pressure on the tendons. A re-alignment of the tendons may then be performed by removing small pieces of bone to straighten the toe. In some cases, the insertion of pins is needed to keep the bones in the proper position as the toe heals. The patient is usually allowed to return home on the same day as the surgery.
If surgery is performed to repair a hammertoe, following the postoperative directions of your doctor is essential. Directions may include several stretches, picking up marbles with your toes, or attempting to crumple a towel placed flat against your feet. Wear shoes that have low heels and a wide amount of toe space to maintain comfort. Closed-toe shoes and high heels should be avoided. Shoes with laces allow the wearer to adjust how fitted he or she may want the shoes to be and also allow for greater comfort. To provide adequate space for your toes, select shoes that have a minimum of one-half inch of space between the tip of your longest toe and the inside of the shoe. This will also relieve pressure on your toes and prevent future hammertoes from forming.
Other preventative measures that can be taken include going shopping for new shoes in the middle of the day. Your feet are its smallest in the morning and swell as the day progresses. Trying on and purchasing new shoes midday will give you the most reliable size. Be sure to check that the shoes you purchase are both the same size. If possible, ask the store to stretch out the shoes at its painful points to allow for optimum comfort.
Why Do I Have Hammertoes?
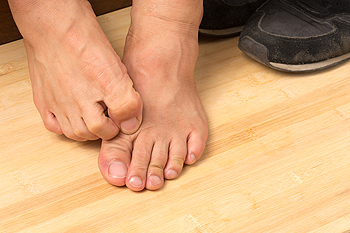
 Hammertoes are a type of toe deformity that cause the ends of the affected toes to bend downward at the middle joint. At first, the affected toes may be flexible, but over time, the joints can become stiff, leaving the toes stuck in a claw-like position. The most common cause of hammertoes is wearing shoes that are too narrow and tight, which cause the toes to bend upward. Muscles and tendons within the affected toes become tighter and shorter, causing the toe to remain in a bent position long after you have taken off the shoes. Risk factors that increase your risk of developing hammertoes also include having longer toes, bunions, or rheumatoid arthritis. Hammertoes can cause pain and discomfort, make it difficult to wear shoes, and increase your chances of getting corns, calluses, and blisters on your toes. If you have hammertoes, it is suggested that you seek the care of a podiatrist.
Hammertoes are a type of toe deformity that cause the ends of the affected toes to bend downward at the middle joint. At first, the affected toes may be flexible, but over time, the joints can become stiff, leaving the toes stuck in a claw-like position. The most common cause of hammertoes is wearing shoes that are too narrow and tight, which cause the toes to bend upward. Muscles and tendons within the affected toes become tighter and shorter, causing the toe to remain in a bent position long after you have taken off the shoes. Risk factors that increase your risk of developing hammertoes also include having longer toes, bunions, or rheumatoid arthritis. Hammertoes can cause pain and discomfort, make it difficult to wear shoes, and increase your chances of getting corns, calluses, and blisters on your toes. If you have hammertoes, it is suggested that you seek the care of a podiatrist.
Hammertoe
Hammertoes can be a painful condition to live with. For more information, contact Dr. Thomas Madden from Advanced Foot Care Center. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe is a foot deformity that affects the joints of the second, third, fourth, or fifth toes of your feet. It is a painful foot condition in which these toes curl and arch up, which can often lead to pain when wearing footwear.
Symptoms
- Pain in the affected toes
- Development of corns or calluses due to friction
- Inflammation
- Redness
- Contracture of the toes
Causes
Genetics – People who are genetically predisposed to hammertoe are often more susceptible
Arthritis – Because arthritis affects the joints in your toes, further deformities stemming from arthritis can occur
Trauma – Direct trauma to the toes could potentially lead to hammertoe
Ill-fitting shoes – Undue pressure on the front of the toes from ill-fitting shoes can potentially lead to the development of hammertoe
Treatment
Orthotics – Custom made inserts can be used to help relieve pressure placed on the toes and therefore relieve some of the pain associated with it
Medications – Oral medications such as anti-inflammatories or NSAIDs could be used to treat the pain and inflammation hammertoes causes. Injections of corticosteroids are also sometimes used
Surgery – In more severe cases where the hammertoes have become more rigid, foot surgery is a potential option
If you have any questions please contact our office located in Killeen, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is a Podiatrist?
The branch of medicine that is focused on the treatment, diagnosis, and study of disorders of the lower leg, ankle and foot is referred to as podiatry. Because people often spend a great deal of their time on their feet, many problems in this area can occur. A person seeks help from the field of podiatry when they need treatment for heel spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, infections, and problems with the foot that are related to diabetes and additional diseases.
To treat problems of the foot, ankle or lower leg, a podiatrist may prescribe physical therapy, drugs, perform surgery, or set fractures. Individuals may also be recommended to wear corrective shoe inserts, custom-made shoes, plaster casts and strappings in order to correct deformities.
When trying to gather information on a patient problem, a scanner or force plate may be used in order to design orthotics. During this procedure, patients are told to walk across a plate that is connected to a computer; the computer then takes a scan of the foot and indicates weight distribution and pressure points. The computer readouts will give the podiatrist information to help them determine the correct treatment plans.
Diagnosis is also provided through laboratory tests and x-rays. Through the foot, the first signs of serious problems such as heart disease, diabetes and arthritis can show up. For example, individuals that have diabetes may frequently have problems such as infections and foot ulcers because they experience poor circulation in the foot area. A podiatrist can then have consultations with patients when symptoms arise. Referrals will then be made to specialists that handle the greater health problems.
Some podiatrists have their own independent, private practices or clinics where they have a small staff and administrative personnel. Many podiatrists work within group practices. They usually spend time performing surgery in ambulatory surgical centers or hospitals, or visit patients in nursing homes. Podiatrists typically spend between 30 to 60 hours of week working. Some podiatrists specialize in public health, orthopedics, surgery, or primary care. Other fields include specialties in geriatrics, dermatology, pediatrics, diabetic foot care and sports medicine.
Some podiatrist specialists complete extra training in the area of foot and ankle reconstruction that results from the effects of physical trauma or diabetes. There are also surgeons that perform surgery of a cosmetic nature to correct bunions and hammertoes.
Why Should I Visit a Podiatrist?
 Podiatrists provide a wide range of medical care for any issues pertaining to the feet and ankles. Podiatrists are able to diagnose, treat, and in some cases even provide surgery for specific ailments. Due to the wide range of services, there are many reasons to visit a podiatrist. Those who are feeling joint pain in the feet or ankles may be suffering from arthritis and will need to see a podiatrist. Diabetics are very susceptible to foot wounds and should be under the care of a podiatrist to avoid amputation with severe cases of foot ulcers. You may experience heel pain and a proper diagnosis is the first step toward developing the correct treatment plan. They are also experts in caring for broken or sprained feet, ankles, and toes. If you are suffering from any foot or ankle condition, don’t hesitate to reach out to your podiatrist today!
Podiatrists provide a wide range of medical care for any issues pertaining to the feet and ankles. Podiatrists are able to diagnose, treat, and in some cases even provide surgery for specific ailments. Due to the wide range of services, there are many reasons to visit a podiatrist. Those who are feeling joint pain in the feet or ankles may be suffering from arthritis and will need to see a podiatrist. Diabetics are very susceptible to foot wounds and should be under the care of a podiatrist to avoid amputation with severe cases of foot ulcers. You may experience heel pain and a proper diagnosis is the first step toward developing the correct treatment plan. They are also experts in caring for broken or sprained feet, ankles, and toes. If you are suffering from any foot or ankle condition, don’t hesitate to reach out to your podiatrist today!
If you are dealing with pain in your feet and ankles, you may want to seek help from a podiatrist. Feel free to contact Dr. Thomas Madden from Advanced Foot Care Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
A podiatrist is a doctor of podiatric medicine who diagnoses and treats conditions of the foot, ankle, and related structures of the leg. Your podiatrist may specialize in a certain field such as sports medicine, wound care, pediatrics, and diabetic care. Podiatrists have the ability to become board certified through training, clinical experience, and then taking an exam.
What Do Podiatrists Do?
On a daily basis, a podiatrist may perform the following activities:
- Diagnose foot ailments such as ulcers, tumors, fractures, etc.
- Use innovative methods to treat conditions
- Use corrective orthotics, casts, and strappings to correct deformities
- Correct walking patterns and balance
- Provide individual consultations to patients
It is very important that you take care of your feet. It’s easy to take having healthy feet for granted, however foot problems tend to be among the most common health conditions. Podiatrists can help diagnose and treat a variety of feet related conditions, so it is crucial that you visit one if you need assistance.
If you have any questions please feel free to contact our office located in Killeen, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
What You Need to Know to Prevent Diabetic Foot Ulcers
People with diabetes are prone to developing diabetic foot ulcers, sores on the feet that can heal very slowly or may never heal at all. About 5% of people with diabetes develop chronic foot ulcers, which can cause complications such as infection and amputation. Preventing diabetic foot ulcers is of the utmost importance. If you have diabetes, it is necessary to know how to manage your condition. You should be aware of the medications that you take and their dosages, eat a balanced diet, take any prescribed supplements, see your doctor regularly, and monitor your foot health. A podiatrist can teach you how to perform daily foot checks to identify any cuts, scrapes, sores, or wounds on your feet early. The earlier these things are detected, the better they respond to treatment. A podiatrist can also teach you how to care for foot wounds at home. For more information about diabetic foot wounds, please speak with a podiatrist.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Thomas Madden from Advanced Foot Care Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Killeen, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
Athlete's Foot Symptoms
Athlete’s foot refers to a fungal infection of the skin on the feet. While the infection is common among athletes, you don’t have to be one to get it. Athlete’s foot is contagious and spreads through direct contact between the fungus and your skin. You can pick up this infection from walking barefoot in public spaces, particularly in warm, moist environments such as locker rooms and swimming pools, or from sharing personal items such as towels and socks. Athlete’s foot has several noticeable symptoms, including an itching, stinging, or burning sensation between the toes or on the soles, and dry, cracking, peeling, or raw skin on the feet. Often this infection can spread to the toenails, causing them to become discolored, thick, and crumbly. If you have symptoms of athlete’s foot, it is suggested that you see a podiatrist for treatment.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Dr. Thomas Madden from Advanced Foot Care Center. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our office located in Killeen, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.